Материал: BASIC CLINICAL SYNDROMES IN INTERNAL DESEASES CLINIC
3. Hepatic jaundice (parenchymal)
REASONS: acute and chronic hepatitis, infectious mononucleosis, drug and alcoholic liver lesions, cirrhosis, hepatocellular cancer.
SYMPTOMS:
Dull pain in the right hypochondrium, jaundice, unstable skin itching, general weakness. The skin is saffron yellow with a reddish tint, the liver is enlarged, tightened, often slightly painful, sometimes normal or reduced. Bradycardia
Blood - hyperbilirubinemia, often due to both direct and indirect fractions of bilirubin, a decrease in prothrombin, an increase in the activity of transaminases (ALT, AST).
Urine - dark, beer-colored, bilirubinuria, urobilinuria
Feces - not changed or moderately discolored, the release of stercobilin is reduced.
Instrumental techniques confirm liver damage.
4. Suprahepatic jaundice (hemolytic)
REASONS: congenital or acquired independent diseases (microspherocytic hereditary anemia, neonatal erythroblastosis, acute post-transfusion anemia), or a symptom of a number of diseases (croupous pneumonia, subacute septic endocarditis, Addison-Birmer disease, malaria, lung infarction, malignant tumors, some, or a consequence of toxic and drug damage (arsenic, hydrogen sulfide, phosphorus, sulfonamides).
SYMPTOMS:
General weakness, decreased appetite.
Jaundice without itching with a lemon-yellow tint and pallor of the skin.
The liver is slightly enlarged, painless.
The spleen is enlarged.
In the blood, moderate hyperbilirubinemia, mainly due to free (indirect) bilirubin. Signs of hemolytic anemia. Coombs test is positive.
The indicators ALT, AST are not changed.
In the urine there is no bilirubin, but there is an increased amount of urobilin.
The feces are dark, the content of stercobilin is increased.
68
6. Cholestatic syndrome
stagnation and violation of the secretion of bile into the duodenum with the accumulation of its components in the liver and blood.
Allocate intrahepatic and extrahepatic cholestasis. CAUSES of extrahepatic cholestasis:
1. Stones of the main extrahepatic and main intrahepatic ducts;
2. Damage to the head of the pancreas (tumor, pancreatitis, cyst, abscess);
3. Stenosis and tumor of the large duodenal papilla;
4. Inflammation, tumors and strictures of the extrahepatic bile ducts;
5. Parasitic infections (opisthorchiasis, fascioliasis, ascariasis, clonorchosis, echinococcosis);
6. Enlarged lymph nodes in the gates of the liver;
7. Tumor and duodenal diverticulum. REASONS for intrahepatic cholestasis:
1. acute and chronic hepatitis;
2. Cirrhosis of the liver (especially primary biliary cirrhosis);
Liver tumors, sarcoidosis, tuberculosis, lymphogranulomatosis, cholangitis, pregnant cholestasis, drug cholestasis.
SYMPTOMS:
Itching, pigmentation and scratching of the skin;
Jaundice, enlarged liver;
Xanthomas, xanthelasms;
With prolonged cholestasis - there may be visual disturbances in the dark, bleeding, bone pain (due to malabsorption of fat-soluble vitamins A, E, D, K);
An increase in serum bilirubin (mainly associated), the activity of alkaline phosphatase, gamma-glutamine transferase, leucine aminopeptidase, the level of bile acids, cholesterol and its fractions, copper;
A sharp decrease or disappearance of urobilin in the urine.
Hepatolienal syndrome
REASONS: acute and chronic hepatitis and cirrhosis, acute and chronic leukemia, sepsis, collagenoses, pathology of the liver vessels, infectious diseases (malaria, leptospirosis). SYMPTOMS:
Clinical and instrumental signs of hepatosplenomegaly.
The detection of enlarged liver and spleen allows you to clinically differentiate the diseases associated with this syndrome. Often, it is accompanied by hypersplenism syndromes and liver damage.
8. Hypersplenism syndrome
Hypersplenism is an increase in spleen function.
REASONS: diseases that occur with portal hypertension, hepatitis and cirrhosis of the liver,
accumulation diseases, granulomatosis with enlarged spleen (sarcoidosis, lymphogranulomatosis), diffuse connective tissue diseases, parasitic lesions of the spleen. SIGNS:
anemia;
leukopenia;
thrombocytopenia.
9. Portal hypertension
This is an increase in pressure in the portal vein pool, associated with the presence of an obstruction to the outflow of blood.
REASONS of portal hypertension:
I - prehepatic (subhepatic) portal hypertension:
Thrombosis or occlusion of the portal vein by a tumor or lymph nodes.
Increased portal venous blood flow: arteriovenous fistula, splenomegaly, not associated with liver disease, portal vein cavernomatosis;
II Intrahepatic portal hypertension:
Cirrhosis of the liver, cirrhosis, less commonly veno-occlusive disease, sarcoidosis,
schistosis
III Posthepatic (suprahepatic) portal hypertension:
Hepatic vein thrombosis (Budd-Chiari syndrome), membranous obstruction of the inferior vena cava, constrictive pericarditis, liver fibrosis in congestive heart failure, tumor compression of the inferior vena cava and hepatic veins;
SYMPTOMS: Supporting symptoms: - ascites
- Varicose veins in the system of portocaval anastomoses (cardial sections of the esophagus and stomach, superficial veins of the abdomen, hemorrhoidal veins)
- Esophageal, hemorrhoidal bleeding
- Increased pressure in the portal vein and its expansion (instrumental signs)
Complaints. Decreased appetite, nausea, flatulence, signs of dyspepsia, decreased diuresis. Flatulence often precedes the appearance of ascites. Sometimes, bloody vomiting, stool with blood.
Objectively: clinical signs of ascites (enlarged swollen abdomen, navel protrusion, expansion of the saphenous veins of the abdominal wall - the ―jellyfish head‖, frog stomach, positive symptom of fluctuations, dull percussion sound) often emaciation to cachexia, peripheral edema (edematous ascites may occur) syndrome due to hypo- and dysproteinemia, secondary hyperaldosteronemia).
Sometimes (with the development of collaterals through the umbilical veins), venous noise occurs on the anterior abdominal wall. Noise is especially pronounced in the umbilical region with cirrhosis of the liver in combination with non-closure of the umbilical vein (Crewellier-Baumgarten syndrome).
Blood: dysproteinemia (less often a decrease in the total amount of protein), a decrease in albumin, sometimes positive sedimentary reactions.
Urine - often oliguria.
EFGDS - determined by varicose veins of the lower esophagus and the entrance of the stomach, rectum.
Ultrasound - detected fluid in the abdominal cavity, increased venous pressure in the portal vein and its expansion.
Table 4.1 Ascites fluid:
-
Transudate
Exudate
Specific gravity
lower 1015
above 1018
Protein
lower 30,0 г/л
above 30,0 г/л
Rivalta Test
-
+
70
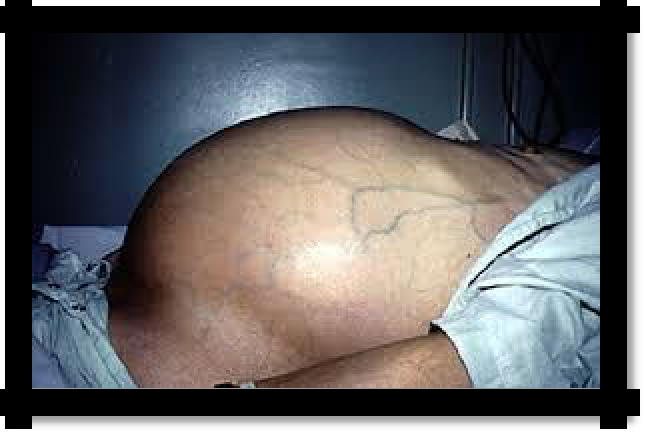
Pic 4.5 Ascites, expansion of superficial veins of the abdomen (head of Medusa).
10. Hepatic failure syndrome
This is a pathological condition accompanied by a violation of the basic functions of the liver
(absorption-excretory, metabolic and synthetic).
CAUSES:
acute diseases and lesions of the liver (acute hepatitis, leptospirosis, alcoholic, toxic and drug hepatitis.
chronic liver disease (chronic hepatitis and cirrhosis of the liver, hemochromatosis, Wilson-Konovalov’s disease, etc.)
malignant tumors of the liver.
small liver failure or hepatosuppressive syndrome (hepatodepression), in which various violations of the liver function develop, but without the development of encephalopathy.
large liver failure (hepatathy, hepatic encephalopathy, hepatocerebral syndrome) - severe liver failure, which is accompanied by hepatic encephalopathy with the subsequent development of coma.
Signs of hepatic encephalopathy:
1. Decreased intelligence, slowing thinking, excitability and euphoria, which are replaced by
depression, drowsiness, auditory and visual hallucinations, memory lapses.
Sometimes tonic cramps, twitching of various muscle groups, a symptom of "clapping tremor".
Tendon and pupillary reflexes are reduced, pathological neurological reflexes appear (Babinsky, Gordon, Rossolimo, etc.).
General weakness, lack of appetite, weight loss.
Hepatic breath.
Jaundice intensifies, the size of the liver decreases (especially in acute liver pathology).
The phenomena of hemorrhagic diathesis are growing.
Ascites, swelling.
The body temperature is increased (in the terminal stage - reduced).
Increased serum ammonia levels.
A hepatic coma develops.
Signs:
1. consciousness is completely lost, do not respond to light;
71
Kussmaul breathing, subsequently - Cheyne-Stokes, Biota;
the stiff neck muscles and limb muscles;
pathological reflexes of Babinsky, Gordon, Zhukovsky, in some cases grasping and proboscis;
Blood pressure is reduced, tachycardia, deafness of heart sounds;
Jaundice is pronounced, the size of the liver is reduced;
Anuria;
Hemorrhagic syndrome is expressed (skin hemorrhages, nose, stomach, intestinal, uterine bleeding);
In the blood: leukocytosis, azotemia, bilirubinemia, lower potassium, cholesterol, lower previously increased activity of ALT, AST, LDH, cholinesterase;
Lowered body temperature;
ECG - hypersynchronous delta waves dominate.
12. Cytolysis syndrome (cytolytic syndrome)
Nonspecific reaction of liver cells to the action of damaging factors (destruction of liver cells). It is based on a change in the permeability of cell membranes and their organs. This leads to the release of the constituent parts of the cells into the intercellular space and into the blood - and the entry of sodium and water into the cell.
REASONS: acute and chronic hepatitis and cirrhosis of various origins, swollen and tumor metastases in the liver, shock of any nature, starvation. SYMPTOMS:
Biochemical parameters: increased activity of ALT, AST, aldolase, iron, bilirubin in blood serum, decreased blood coagulation factors, albumin, cholinesterase activity;
Signs of hepatic cell failure;
Asthenovegetative syndrome;
Dyspeptic syndrome;
Hepatic jaundice syndrome;
Syndrome of endocrine disorders: gynecomastia, decreased libido, testicular atrophy, impaired hair growth;