Материал: MasterPass _ Pharmacology in 7 Days for Medical Students
PHARMACOLOGY IN 7 DAYS FOR MEDICAL STUDENTS
Insulin
Glucose
Glucose Glycogen
Biguanides 

 Glycagon
Glycagon
Gluconeogenesis
H
e
p
a
tocyte
Figure 3.28 Effects of insulin, glucagon and biguanides on hepatocytes
protects itself from the toxic effects of heme by polymerising the heme to non-toxic hemozoin. Chloroquine is also concentrated in the food vacuoles where it binds to heme-polymerase preventing heme polymerisation. Heme accumulation results in oxidative damage to the membranes leading to lysis of the parasite.
It appears that quinidine and mefloquine also have the same mechanism of action.
Artemether
Artemether is a potent antimalarial drug used for the treatment of multi-drug resistant plasmodium falciparum infection and cerebral malaria. It is derived from Qinghaosu plant and has been in use in Chinese medicine since ancient times. Just like chloroquine, this drug preferentially concentrates in the food vacuoles of plasmodium, where it is metabolised to form toxic free radicals. Additionally, it appears that this drug covalently binds to specific malarial proteins, damaging and thus rendering them non-functional.
Artemether
Heme
Artemether-Heme adduct (→ toxic to plasmodia)
Figure 3.29 Mechanism of action of artemether
94
MECHANISMS OF ACTION
Digoxin
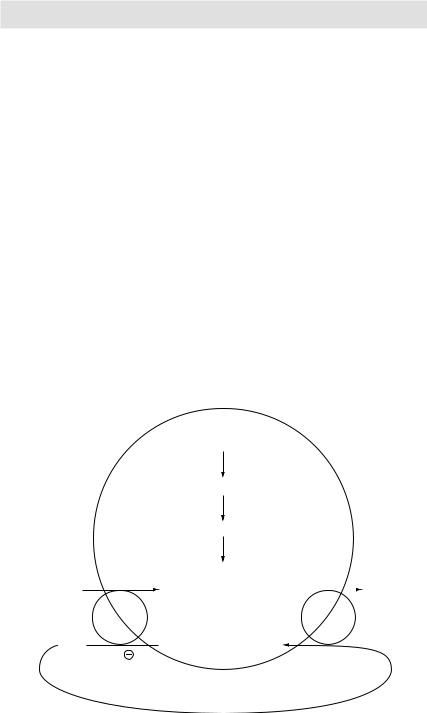
Digoxin, a cardiac glycoside, inhibits the Na+/K+ ATPase pump present in the cell membrane of cardiac myocytes. This pump normally causes Na+ efflux in exchange of K+ influx. A rise in ECF Na+ in turn improves the gradient for Na+ influx via the Na+/Ca++ pump – another cell membrane pump responsible for Na+ influx in exchange of Ca++ efflux. Digoxin, by inhibiting Na+/K+ ATPase pump, in turn decreases the activity of Na+/Ca++ pump. The net effect is a rise in intracellular Ca++ so that when the digoxin-treated myocyte is depolarised, more Ca++ is available to facilitate contraction.
Besides the above-mentioned positive inotropic effect (increased force of contraction), digoxin also exerts a negative chronotropic effect (slowed rate of contraction) by a direct action on the cardiac conduction system. It prolongs the refractory period of AV node and slows the conduction velocity via the node.
Because of the characteristic electrophysiological effects of digoxin on heart, it is the drug of choice in treating atrial fibrillation (AF) in patients who have concomitant left ventricular failure. The aim of drug therapy in most AF patients is to slow the ventricular rate. Digoxin, by virtue of its negative chronotropic effect, achieves this aim, but unlike the other rate-controlling drugs used in AF (like β-blockers or rate-limiting Ca++ channel blockers like verapamil or diltiazem), it doesn’t worsen the left ventricular failure (it increases the force of contraction, whereas other drugs not only decrease the rate of contraction but also the force of contraction).
Digoxin
↓activity of Na+/K+ ATPase pump
↓activity of Na+/Ca++ pump
Na+/K+
ATPase
pump
Na+ 
Digoxin
↑cytosolic Ca++
K+ |
|
|
|
|
|
|
Ca++ |
|
|
|
|
|
|
||
|
|
|
|
|
|
Na+/Ca++ |
|
|
|
|
|
|
|
pump |
|
C |
a |
|
|
|
Na+ |
||
rd |
|
|
s |
||||
|
|
te |
|||||
|
|
y |
|
|
|
||
|
|
|
iac myoc |
|
|
|
|
Figure 3.30 Mechanism of action of digoxin
95
4
Therapeutic uses and side effects
H-1 antagonists: therapeutic uses
1Allergic disorders: Common cold, hayfever, seasonal rhinitis, conjunctivitis, urticaria, angioneurotic oedema, serum sickness, allergic drug reactions.
2Motion sickness (cyclizine, meclizine).
3Ménière’s disease and vertigo.
4Vomiting (promethazine and meclizine); chemotherapy-induced vomiting (diphenhydramine).
H-1 antagonists: side effects
1CNS:
•Sedation is common with the 1st generation antihistamines especially with diphenhydramine and promethazine. Pronounced sedation can occur if other drugs with sedative effect (like benzodiazepines, alcohol) are used concomitantly. Since 2nd generation antihistamines have poor CNS penetration, this side effect is much less common with the newer agents.
2Antimuscarinic effects:
•Like blurred vision, dryness of mouth/respiratory passages, constipation, urinary retention and orthostatic hypotension may occur, especially with some of the 1st generation antihistamines.
3Drug allergy:
•Acute poisoning is common in young children when they are given high doses. It is characterised by atropine-like antimuscarinic side effects.
4Blood dyscrasias:
•Leukopenia, agranulocytosis and haemolytic anaemia.
H-2 antagonists: therapeutic uses
1Peptic ulcer disease (DU, GU, stress ulcers, NSAIDs-induced ulcers): They are also used both in the treatment and prophylaxis of bleeding peptic ulcers.
2GERD.
3Syndromes:
aZollinger-Ellison syndrome (hypergastrinemia → hypersecretion of gastric HCl → besides stomach and duodenum, peptic ulcers also develop at unusual sites like oesophagus and jejunum). Larger doses of H-2 antagonists are required; PPIs are more effective.
96

THERAPEUTIC USES AND SIDE EFFECTS
b Mendelson’s syndrome (acid aspiration syndrome). c Short bowel anastomosis syndrome.
DISCOS:
Digoxin
Isoniazid
Spironolactone
Cimetidine
Oestrogens
Stilboestrol
H-2 antagonists: side effects
1Anti-androgenic: Cimetidine (alone) causes hyperprolactinemia. This in turn may lead to gynecomastia in males and galactorrhea in females.
2Hepatotoxicity: As compared to ranitidine, cimetidine is a potent inhibitor of hepatic drug metabolising enzyme (CYP450). H-2 antagonists also reduce hepatic blood flow.
3Cardiotoxicity: Bradycardia and hypotension.
4Blood dyscrasias: Thrombocytopenia, granulocytopenia and hypoprothrombinemia.
5GIT: Constipation, flatulence and diarrhoea.
6Miscellaneous:
a Opportunistic infections like candidal peritonitis. b Myalgias, arthralgias.
Proton Pump Inhibitors (PPIs): therapeutic uses
1Peptic ulcers (DU, GU, stress ulcers, NSAIDs-induced ulcers): They are also used both in the treatment and prophylaxis of bleeding peptic ulcers.
2GERD.
3Syndromes:
aZollinger Ellison syndrome (hypergastrinemia → hypersecretion of gastric HCl → besides stomach and duodenum, peptic ulcers also develop at unusual
sites like oesophagus and jejunum). PPIs (in high doses) are the most effective and thus preferred drugs in these cases.
b Mendelson’s syndrome (acid aspiration syndrome). c Short bowel anastomosis syndrome.
4 H. pylori (→ peptic ulcers, gastritis, gastric lymphoma) eradication.
Proton Pump Inhibitors: side effects
1 GIT:
a NVD, flatulence and abdominal pain.
bHypergastrinemia (causing rebound hyper-secretion of gastric HCl) after discontinuation of PPI therapy.
cDecreased absorption of vitamin B12 and certain drugs (e.g. digoxin, ketoconazole) that require acidity for their GI absorption.
d Inhibition of hepatic CYP450 enzyme in turn causing decreased metabolism/ clearance of BDZs, warfarin, phenytoin and many other drugs.
2Impotence.
3Gynecomastia.
97

PHARMACOLOGY IN 7 DAYS FOR MEDICAL STUDENTS
4Subacute myopathy and arthralgias.
5Skin rashes.
Laxatives and purgatives: therapeutic uses
1To relieve constipation.
2In pathologies like haemorrhoids and anal fissures.
3Expulsion of parasites after antihelminthic treatment.
4To clear the gut before surgery/endoscopy/radiological examinations (like barium enema).
5To induce labour, e.g. castor oil.
Bulk forming purgatives: therapeutic uses
1Colostomy/ileostomy.
2Constipation due to any cause like anal pathologies, e.g. haemorrhoids, anal fissures; IBD (ulcerative colitis); IBS (irritable bowel syndrome); diverticulitis.
Saline purgatives: therapeutic uses
1Rapid bowel evacuation in 2–3hrs (6.5% solution).
2I/V injection (CNS depressant).
3Injection into the nerve (→ blockade of impulse conduction).
410–20 mL of 20% solution I/M abolishes convulsions.
5Magnesium sulphate and glycerin paste (carbuncles).
650% retention enema (to decrease CSF in neurosurgery).
Bisacodyl: therapeutic uses
1To relieve constipation.
2To evacuate bowel pre-op, before endoscopy or any radiological procedure.
Castor oil: therapeutic uses
1Emollient externally.
2Soother for skin, conjunctiva and nasal mucosa.
3Laxative. Since castor oil delays gastric emptying, it should be given on an empty stomach.
Thiazide diuretics: therapeutic uses
1 Oedema due to:
a Cardiac cause (CCF).
b Hepatic cause (cirrhosis).
c Renal cause (CRF, nephrotic syndrome; acute glomerulonephritis).
2HTN (primary, secondary, pre-eclampsia, i.e. pregnancy-induced hypertension).
3Hypercalciuria (→ recurrent renal stones formation): Thiazide diuretics decrease urinary calcium concentrations and thus are used to prevent renal stone formation.
4Halide poisoning (bromide intoxication).
Mnemonic:
Thiazide diuretics: indications
98